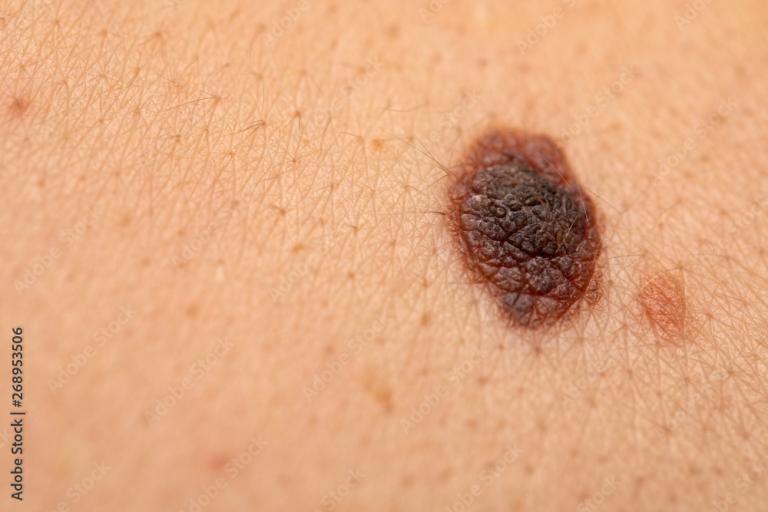
Curing Melanoma with Surgery
A wide local excision of a melanoma will minimise recurrence and will assist with determining the need for additional surgery and ongoing management.
It is common to have one or more surgical drains after lymph node surgery (except sentinel lymph node biopsy) and advice will be given to you as to how long these will be in place and how they are to be managed in the post-operative setting. If you need to go home with drains in place, then at-home nursing visits may be part of your post-operative management to make the recovery process easier.