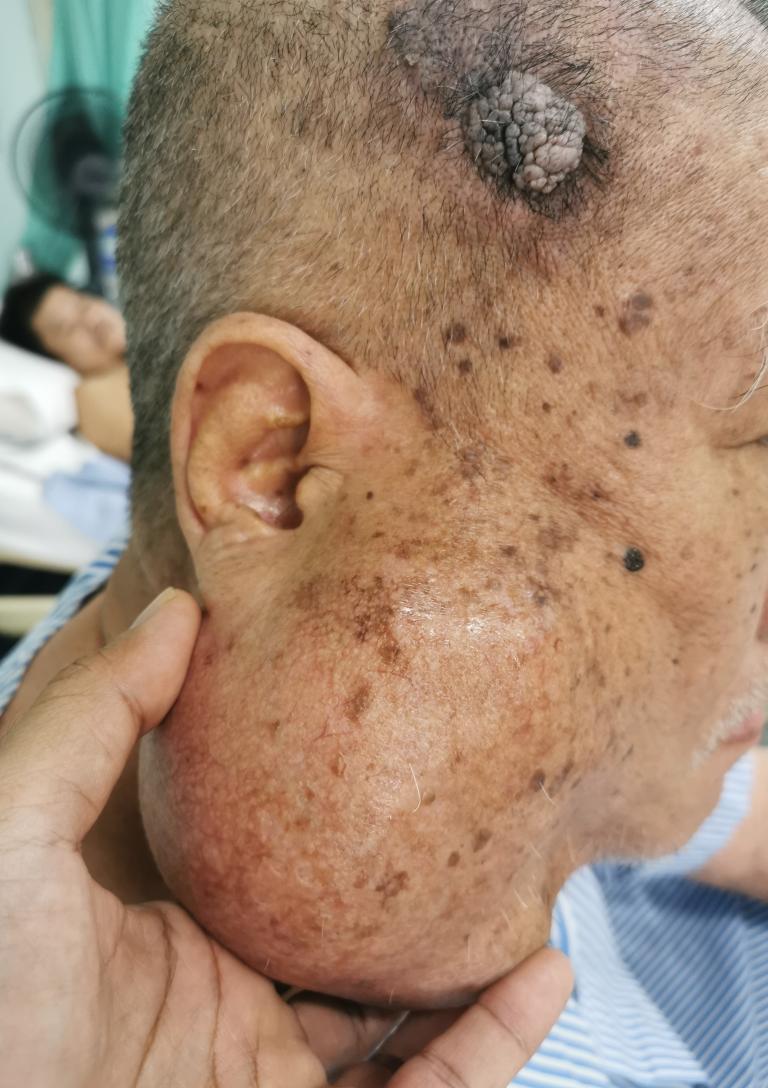
How are Tumours Removed During a Parotidectomy?
A superficial parotidectomy is undertaken to treat tumours and is completed under general anaesthetic.
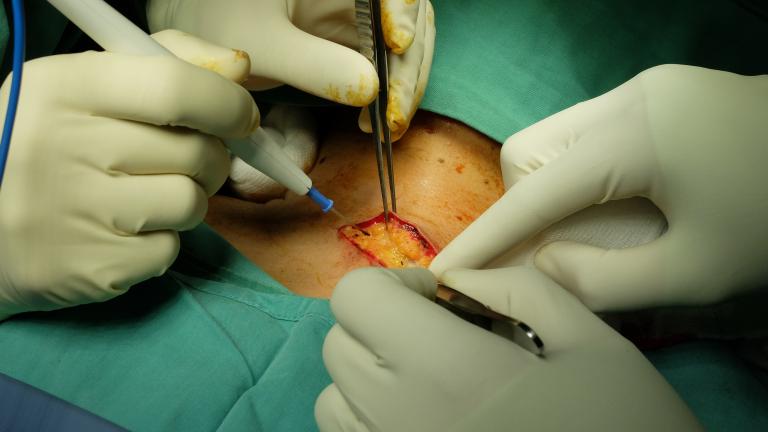
During a parotidectomy, a surgeon begins by making a cut from in front of and below the ear. The surgeon will locate the facial nerve, which passes right through the middle of the parotid gland.
Using a nerve monitoring device, the surgeon carefully follows the nerve through the gland so not to damage it. This nerve controls the muscles that allow you to smile and frown, blink and close the eyes and close the lips.
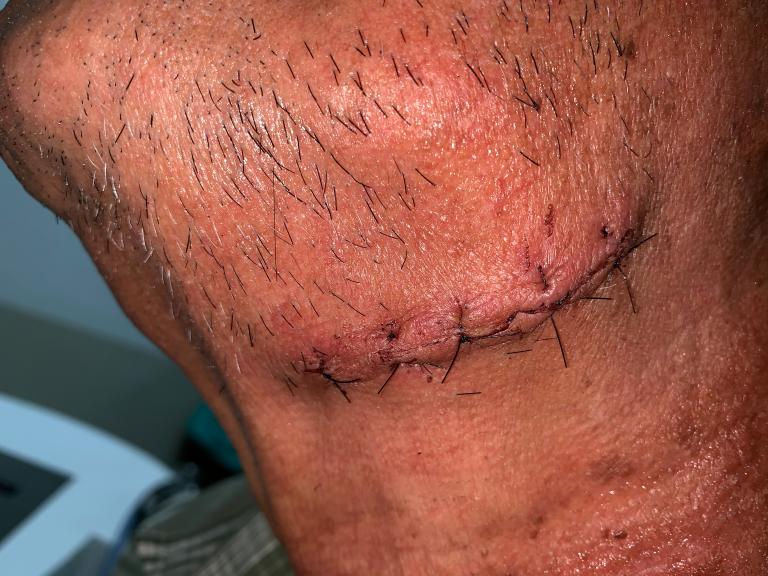
Part or all of the gland is removed, depending on its condition, and the surgeon stitches up the incision and a drain is inserted.
Benign parotid tumours must be completely removed. In more serious cases, the facial nerve will also need to be removed, causing permanent weakness of the facial muscles – also known as facial palsy.
Radiotherapy may follow when cancer is present in the parotid gland, as well as outpatient follow-up.