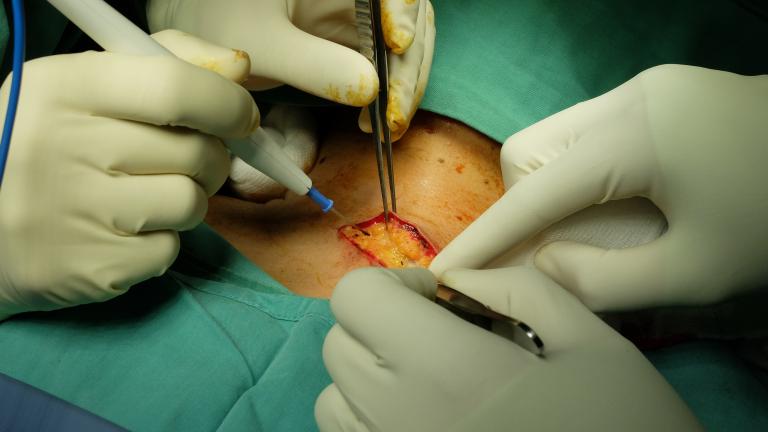
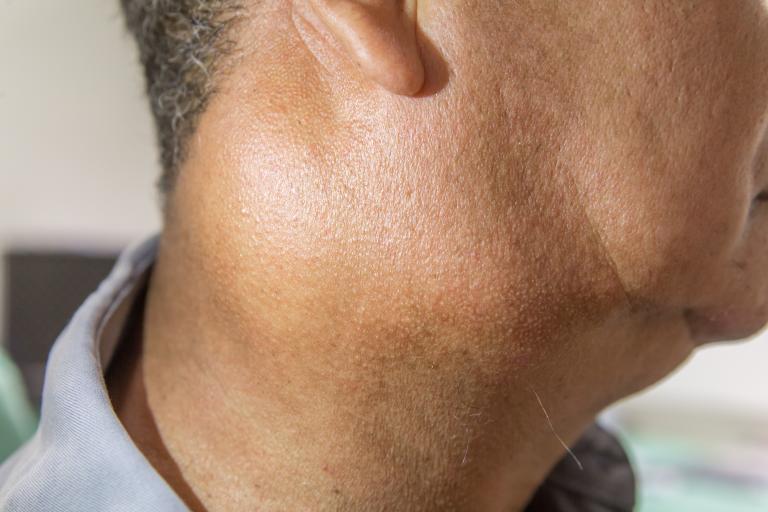
The extent of tissue removal depends on many factors including, the stage of disease which reflects the extent of cancer as well as the type of cancer. The most common cancers removed from lymph nodes in the neck include head and neck squamous cell carcinomas, skin cancers including melanoma and thyroid cancers.. In general, the goal of neck dissection is to remove all the lymph nodes within a predefined anatomic area. Many of the lymph nodes removed during surgery will not prove to have cancer in them.