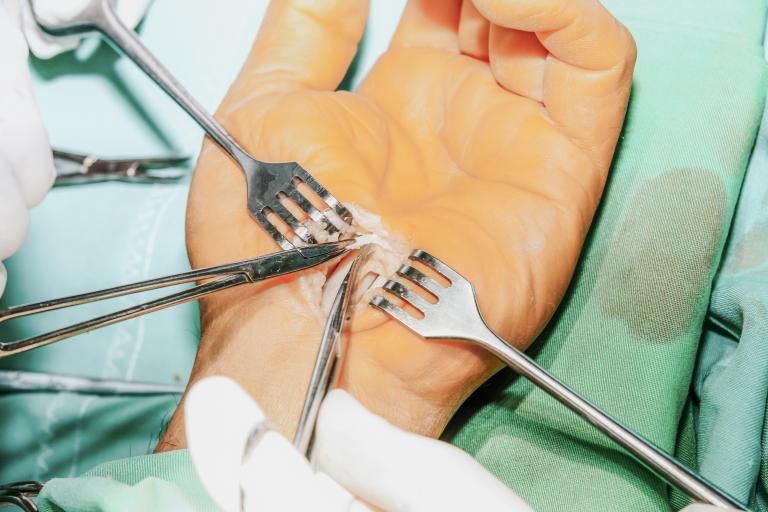
What are the Symptoms of Carpal Tunnel Syndrome?
Pressure on the median nerve in the carpal tunnel can cause symptoms such as tingling in the hand, numbness, a decrease in function or aching. The tendency towards carpal tunnel syndrome may be present in some families. Carpal tunnel symptoms may develop slowly over time but may accelerate after an injury, during pregnancy, as a consequence of diseases such as rheumatoid arthritis and with repetitive use.
Sometimes medications like anti-inflammatories or splinting the hand will relieve the problem, however if this treatment isn’t successful you may require surgery. Carpal tunnel release is best performed before numbness and weakness are present all of the time, but surgery can help prevent worsening of symptoms at any stage of the condition.