What is Reconstructive Plastic Surgery After Trauma?
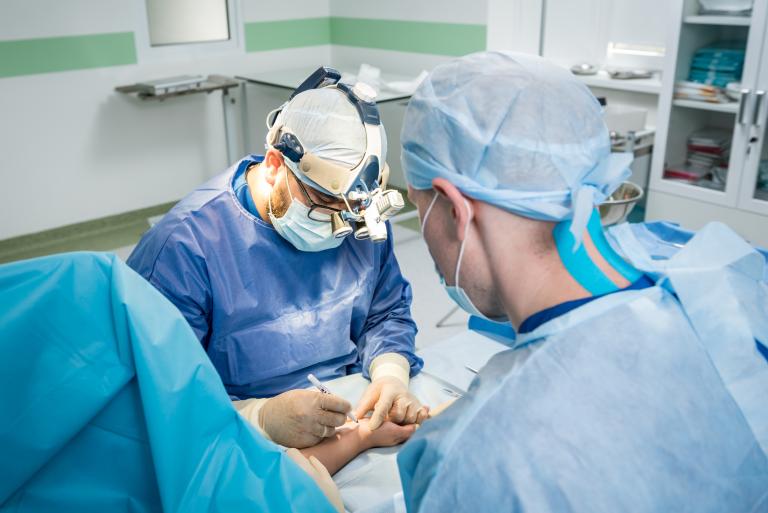
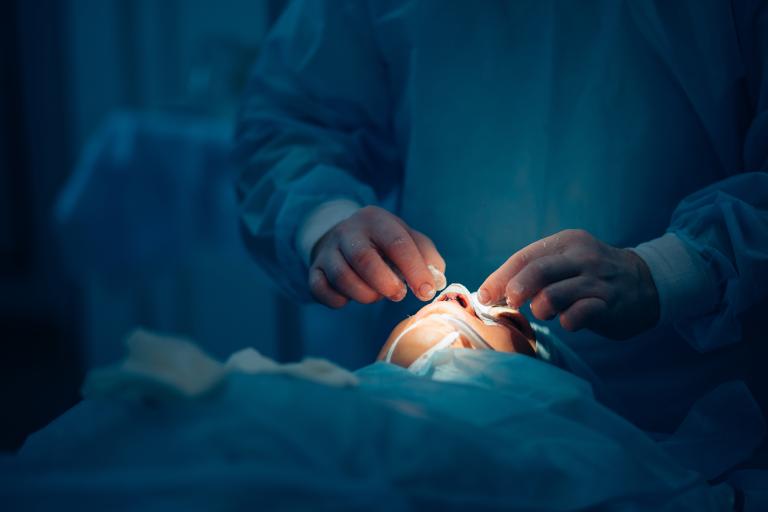
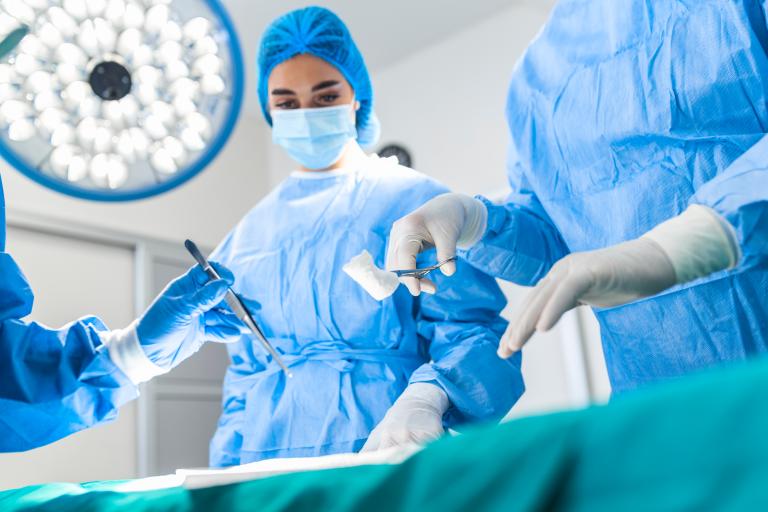
Reconstructive Surgery seeks to repair injured specialised tissues such as tendons, nerve, arteries/veins and bones to permit normal healing. Where tissue is lost due to trauma or infection, it may be necessary to transfer tissue from other parts of the body to allow healing. Additional surgeries are often necessary, sometimes in partnership with Orthopaedic surgeons to remove or replace plates, rods or replacement joints and these require good skin and soft tissue coverage for prompt healing and rehabilitation. It may also be necessary to undertake nerve and muscle transfers to help improve function. We follow our trauma patients for as long as needed to ensure that they are on a good pathway to healing and return of function